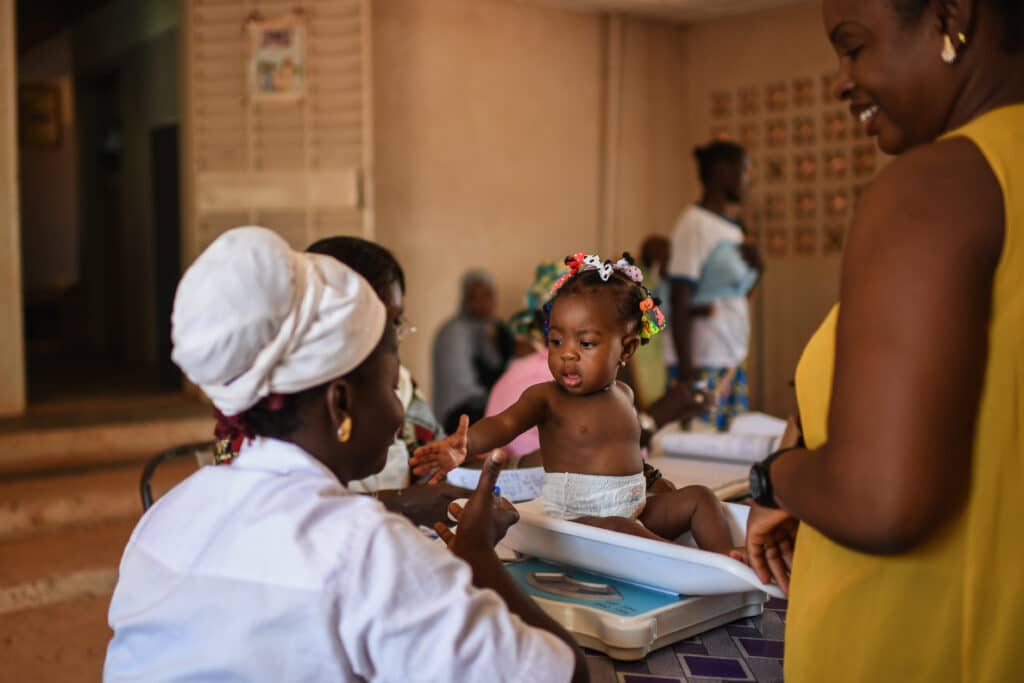
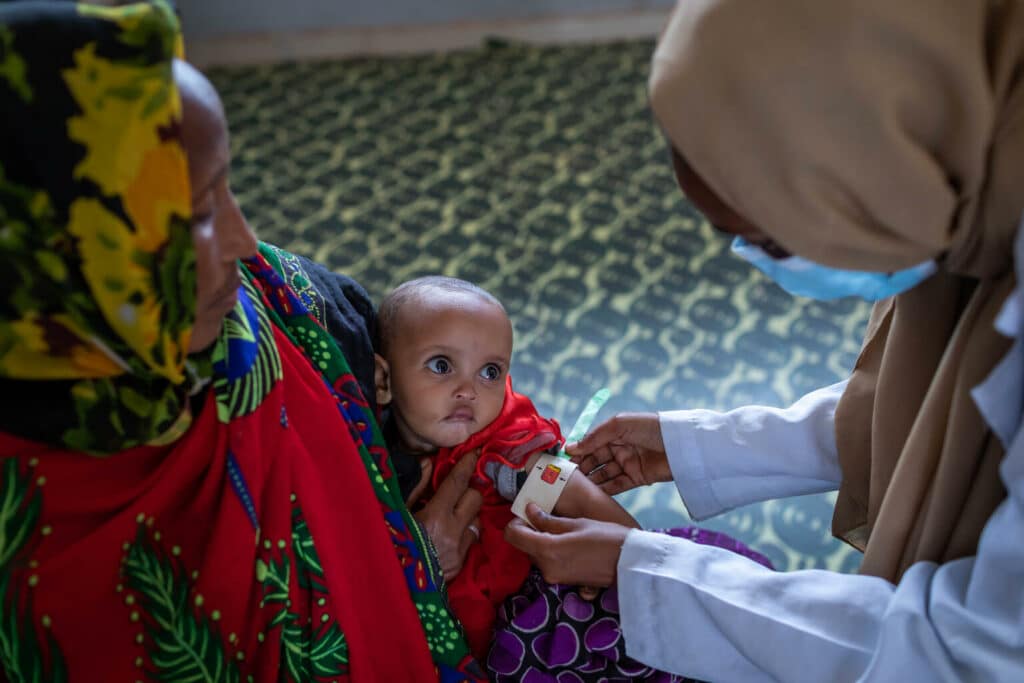
From national policies to ensure breastfeeding is easier to sustain, to targeted support at the individual level, action is required to achieve progress on breastfeeding globally. Breastfeeding counseling – including support for pregnant women and mothers to establish the knowledge, skills, and confidence needed to breastfeed and respond to breastfeeding challenges – is one of the most effective interventions to support women to achieve their breastfeeding goals. However, coverage rates remain low across most low- and middle-income countries (LMICs).
In recognition of 2022 World Breastfeeding Week, focused on increasing education and support for breastfeeding, the ECF team reflects on the state of breastfeeding counseling and how our community can ensure pregnant women and moms worldwide have access to the care they need.

Breastfeeding counseling is a proven cost-effective, scalable solution to fight malnutrition.
A strong body of research shows that breastfeeding counseling is highly effective in promoting exclusive breastfeeding both up to and following the first 6 months of a child’s life.¹ Counseling can help ensure mothers have the support they need to reach their breastfeeding goals, can help them attain skills and confidence along their breastfeeding journey, and can assist with navigating specific challenges – for example, providing advice to mothers on how to sustain their milk supply when returning to work, despite the physiological and logistical challenges this transition can pose.
Breastfeeding counseling is also one of the most cost-effective nutrition interventions. For this reason, in 2018, WHO released global guidance that recommends breastfeeding counseling for all women starting during pregnancy up until the child is two years or older, and defines both expected services and staff expertise required to deliver high-quality breastfeeding counseling.
Though benefits of breastfeeding counseling are widely known, coverage is unacceptably low.
Breastfeeding support is one of four proven, simple solutions – also known as the ‘Power 4’ – to prevent and treat deadly malnutrition alongside delivery of prenatal vitamins, vitamin A supplementation (VAS), and emergency therapeutic foods. These are some of the most cost-effective tools available in global health and development, yet these essential nutrition interventions have extremely low rates of coverage across most LMICs and do not reach the majority of infants, children, and women who need them.
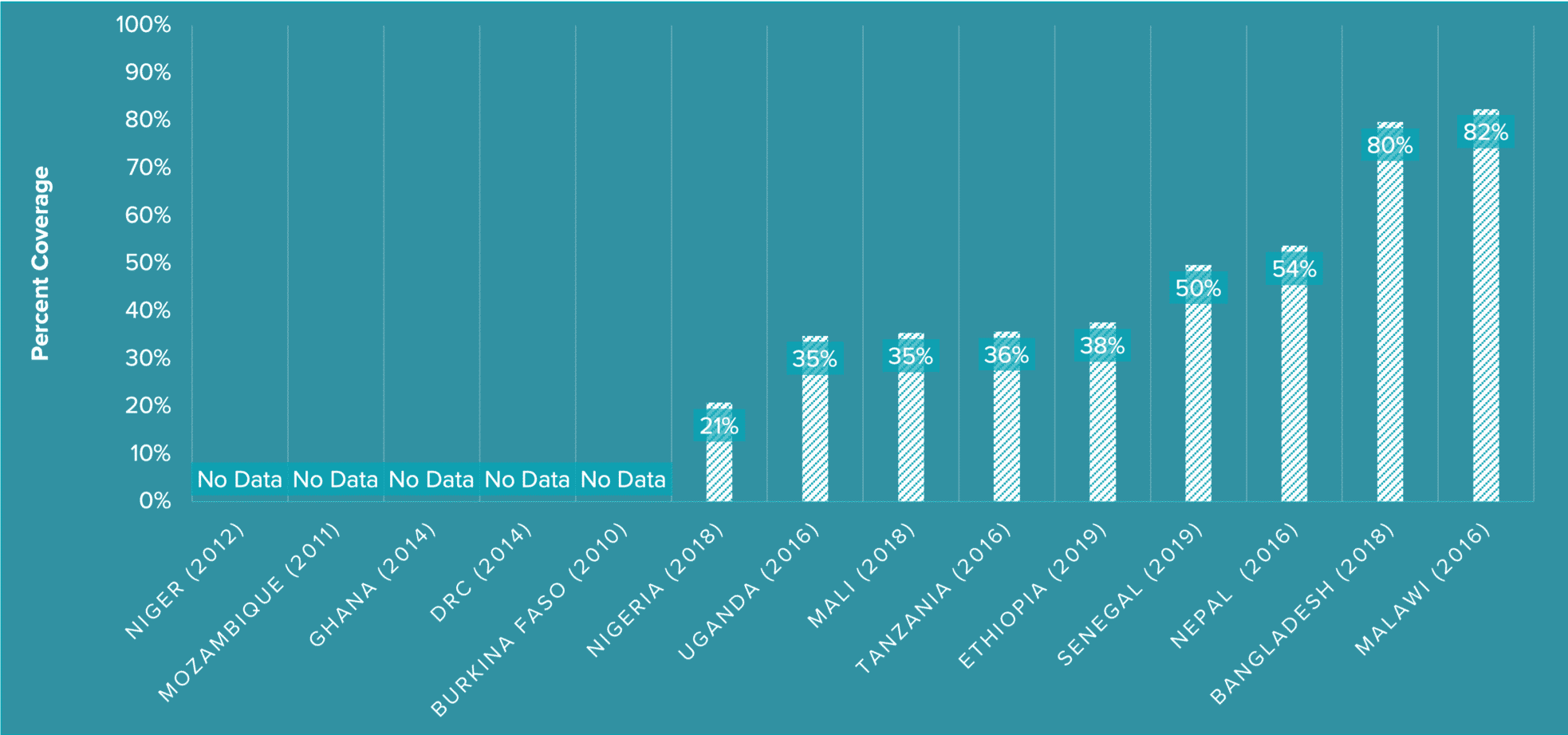
Results for Development recently analyzed coverage of the Power 4 interventions across USAID’s 14 nutrition priority countries (see Figure 1). For breastfeeding counseling, findings show that five countries did not yet have data on coverage, particularly in the two days after delivery. In nine countries which did report data, the coverage of breastfeeding counseling is low with a median of 38%. In Nigeria – which has the most number of children born each year in Africa (and third highest in the world) – the counseling coverage is even worse at 21%.
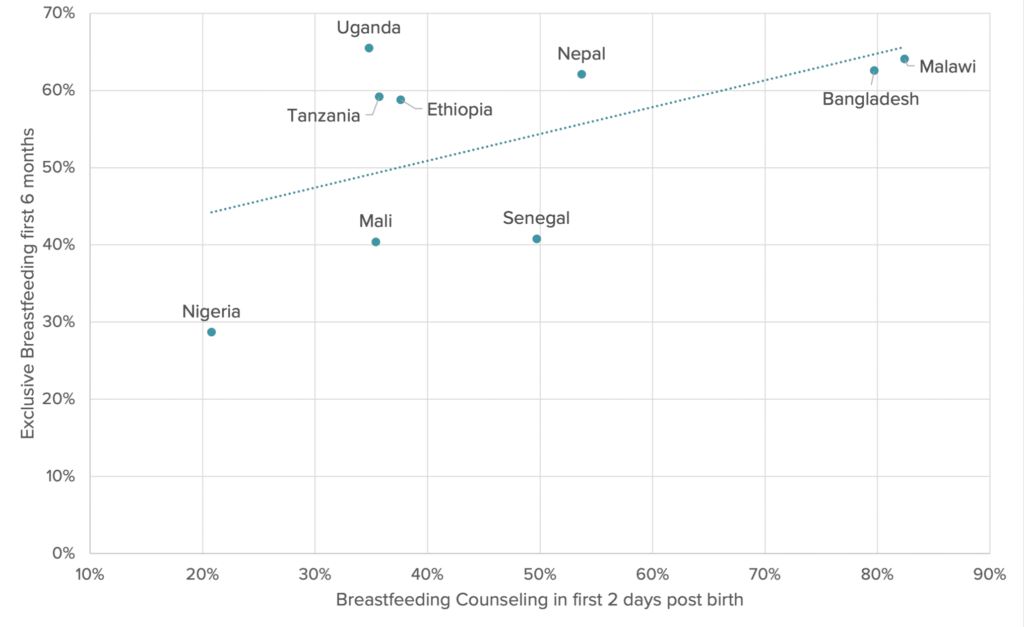
There is a clear association in the data between low coverage of counseling during the first two days after delivery and low rates of exclusive breastfeeding at six months, as seen in Figure 2. This reinforces the key policy point: while a range of interventions and policies may be needed to fully reach national targets, countries struggling with low rates of exclusive breastfeeding may see substantial impact if they scale up coverage of breastfeeding counseling in the first two days post birth. There is also a need for more actionable data on breastfeeding counseling at other critical stages, such as during antenatal care and in the first month after delivery. While one might assume that countries with low coverage of breastfeeding counseling in the first two days also have low coverage of counseling later on, more data is needed to come to that conclusion.²
We can achieve immediate progress on breastfeeding in some countries, by ensuring postnatal care includes breastfeeding counseling.
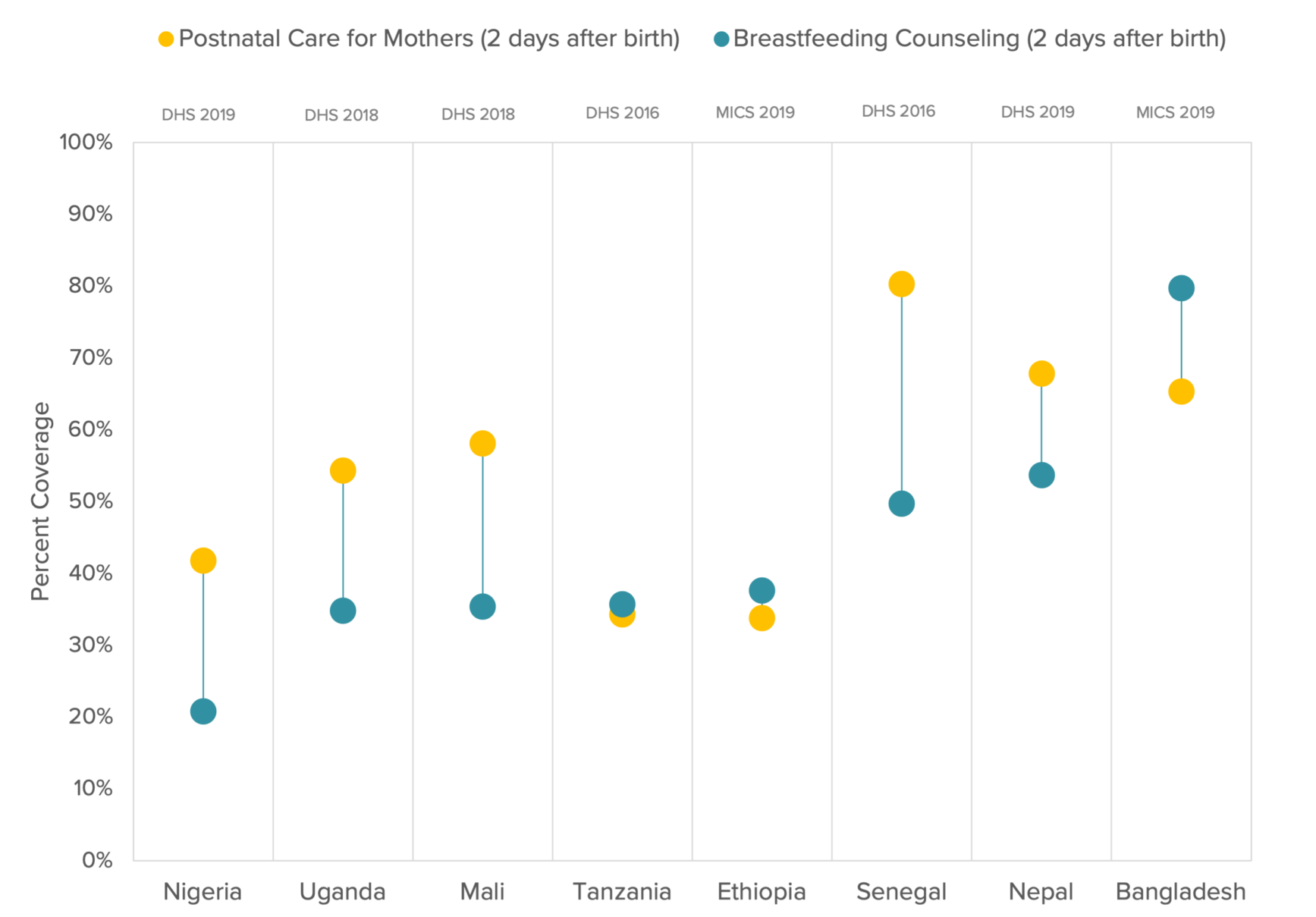
Multiple approaches are needed to scale counseling and improve breastfeeding rates globally. WHO recommends new mothers should receive a basic package of care, including postnatal care which includes the promotion and support of exclusive breastfeeding and the early initiation of breastfeeding. However, as shown in Figure 3 below, in Nigeria, Uganda, Mali, Senegal and Nepal, many women who receive postnatal care in these countries do not receive breastfeeding counseling as part of it. This indicates a clear opportunity to raise breastfeeding counseling coverage in these countries by closing the ‘implementation gap’ within postnatal care. (In contrast, this may be less of an immediate opportunity in countries such as Tanzania and Ethiopia, where postnatal care rates are low, and no higher than breastfeeding counseling rates.)
To close the implementation gap, all healthcare providers and community health workers who interact with mothers should receive training in breastfeeding counseling, and work to integrate counseling into the delivery of other health services. Ministries of Health, policy makers and other government leaders should ensure WHO guidelines on breastfeeding counseling, in addition to basic education and training for healthcare workers, are properly integrated into national strategies for antenatal and postnatal care.
The Eleanor Crook Foundation supports research, policy, advocacy, and communications efforts to integrate the Power 4 interventions – including breastfeeding counseling – into national and local primary health systems, including community health worker protocols.
Our goal is to advocate for and support the strengthening of quality of antenatal and postnatal care to ensure mothers and babies are receiving critical care and have the best chance at healthy lives. Women need and deserve support to reach their breastfeeding goals, and scaling breastfeeding counseling is one of the critical pathways to achieve this.
During this year’s World Breastfeeding Week, we join with our partners to call for the protection, promotion and support of breastfeeding across the globe. By scaling up breastfeeding counseling, with a focus on country contexts and country government priorities, our community could accelerate progress in the fight against malnutrition and save hundreds of thousands of children’s lives.

¹ Bhutta ZA, Ahmed T, Black RE, Cousens S, Dewey K, Giugliani E, Haider BA, Kirkwood B, Morris SS, Sachdev HP, Shekar M; Maternal and Child Undernutrition Study Group. What works? Interventions for maternal and child undernutrition and survival. Lancet. 2008 Feb 2;371(9610):417-40. doi: 10.1016/S0140-6736(07)61693-6. PMID: 18206226.; Kavle, J., LaCroix, E., Dau, H., & Engmann, C. (2017). Addressing barriers to exclusive breast-feeding in low- and middle-income countries: A systematic review and programmatic implications. Public Health Nutrition,20(17), 3120-3134. doi:10.1017/S1368980017002531
² Questions on coverage of breastfeeding counseling during early postnatal care were only added to the demographic and health surveys and multiple indicator cluster surveys in 2015. In addition, existing data on breastfeeding counseling does not provide us with an assessment of the quality of counseling provided and location. https://datadent.org/2019/03/04/breastfeeding-counseling-the-need-for-actionable-data/#_ftn1
Photo Credits © UNICEF/UN0161697, UNICEF/UNI259415, UNICEF/UN0233400/Mawa