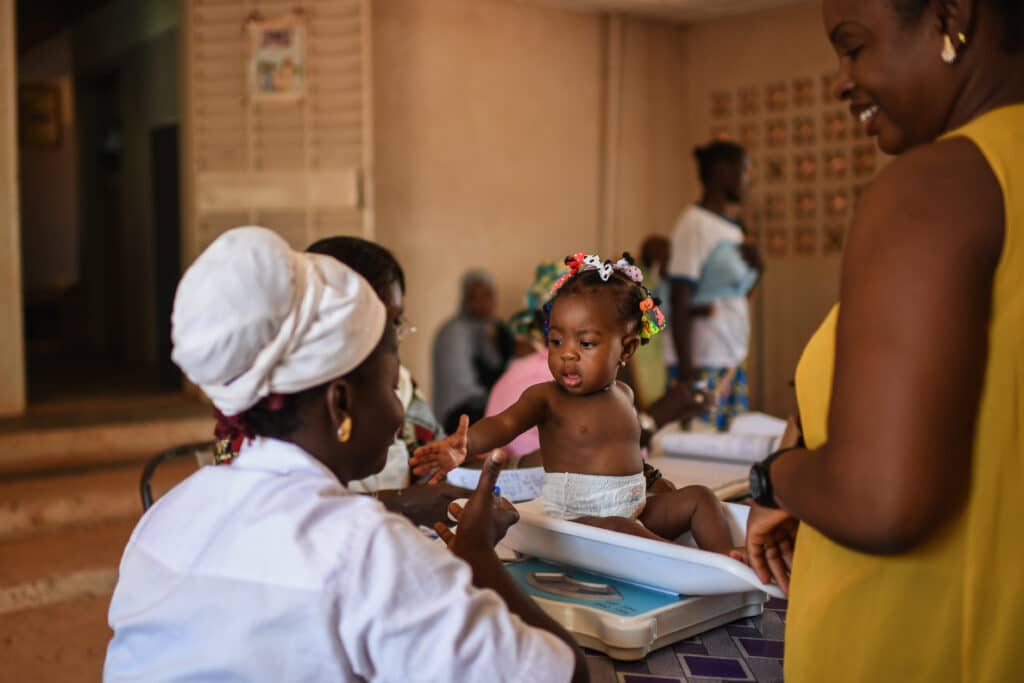
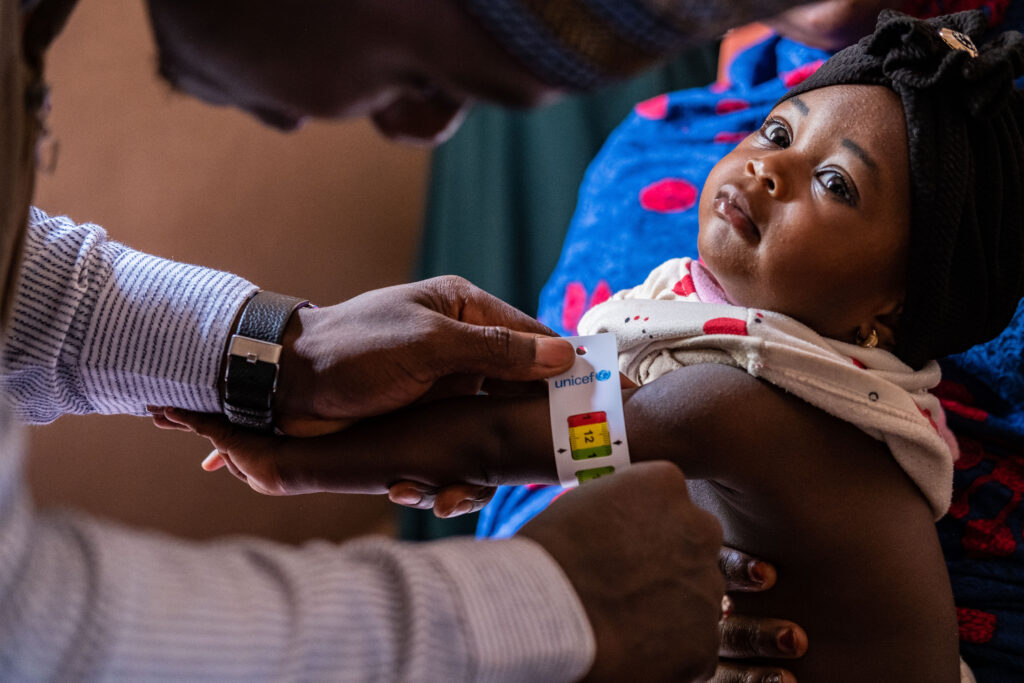
This summer and fall, the World Health Organization (WHO) announced updated recommendations on the treatment and prevention of child wasting.
The updated wasting treatment recommendations were released on July 7, 2023, by WHO as part of a broader guideline update on the Prevention and Management of Wasting and Nutrition Oedema. These revised guidelines reflect years of research on more economical and effective ways to provide treatment for children suffering from wasting. If implemented by national governments and implementing partners, these recommendations offer a path to reach even more children with lifesaving care.
WHO routinely issues guidelines related to clinical practice or public health policy. National governments and implementing partners look to WHO guidelines to inform national policy and practice, and to ensure the most appropriate care and services. The guidelines on child wasting inform the delivery of lifesaving care to children suffering from severe malnutrition, including with ready-to-use therapeutic food (RUTF).
The previous guidelines were issued in 2013. But the last decade of research on the prevention and treatment of wasting has been transformative, including on best practices for expanded delivery platforms, support for infants under six months who are at risk for malnutrition, how to diagnose and treat children suffering from moderate wasting, and optimization of RUTF doses.
The new wasting guidelines have come at a crucial moment. Globally, around 45 million children are currently suffering from wasting.[1] Wasted children are 12 times more likely to die than their well-nourished peers, and are at risk for suffering long-term impacts on their health and development that can cause irrevocable damage. Over the last three years, COVID-19, the effects of climate change, conflict, the global food crisis, and global economic volatility have made the situation worse for the world’s most vulnerable. Earlier this year, five UN agencies released a joint news release calling for urgent action to protect children in 15 countries hit hardest by an unprecedented food and nutrition crisis.
Four components of the wasting treatment guidelines are striking for their potential impact on vulnerable children:
In appropriate contexts, WHO recommends empowering community health workers (CHWs) to identify and treat children with severe wasting at the community level.
Current protocols for wasting treatment center largely on treatment through health facilities, and for millions of children whose lives are threatened by severe wasting, receiving proper treatment requires repeated trips to the nearest health facility — often over long distances, through difficult conditions, and at significant risk and opportunity costs for struggling families (learn more about difficulties accessing wasting treatment here).
As a result of these current protocols, wasted children often are unable to access the lifesaving treatment they need. But evidence suggests that in appropriate contexts, many cases of wasting can be treated safely and effectively by adequately trained and supported CHWs at the community level, eliminating the weekly need to travel long distances to the health facility for most cases. Research shows that this change in protocol will increase coverage of treatment.
Greater focus on infants under six months
WHO guidance on infants under six months have been limited to-date – despite this group being in the most danger from suffering from malnutrition and adverse health outcomes. As a result, caregivers often had to wait for their babies to reach six months of age before receiving comprehensive services, including screening for wasting and treatment as needed.
The new recommendations offer guidelines to support vulnerable infants, including broader admission criteria and regular health check-ups for infants prior to their six-month birthday so that any change in a baby’s weight or health can be caught early. The guidelines also include a focus on maternal well-being. Many of these new recommendations are reflected in the MAMI Care Pathway, which is currently being evaluated in an ECF-funded trial led by The London School of Hygiene & Tropical Medicine.
Guidance on management of moderate wasting
Children who are diagnosed with “moderate wasting” are at a high risk for both stunting and severe wasting – and are thus at a higher risk of death than their well-nourished peers. Globally, more children fall into the category of “moderate” wasting than “severe” wasting. And yet until now, no WHO guidance existed on which cases of child wasting should be prioritized for treatment and how they should be treated. While many national governments and implementing partners developed their own guidance, this patchwork approach has meant that, in practice, children with moderate wasting are often unable to access treatment until their condition has deteriorated into “severe wasting.”
The new guidelines provide recommendations for moderately wasted children. This change means that health systems will have new tools to support children who fall into the category of “high-risk moderate wasting.” More children’s lives will be saved now that they can receive treatment coupled with healthy home foods before they deteriorate further and become severely wasted – and potentially die.
Reduced dosage of Ready-to-Use Therapeutic Food (RUTF)
Current protocols reflect a standard, weight-based dosage system to determine how many sachets of RUTF should be given to a child suffering from severe wasting. But emerging evidence from multiple trials of alternative protocols show that children can receive 30%-40% less RUTF over the course of treatment and still fully recover.
The new guidelines respond to this emerging evidence, and offer insights on how and when health workers can safely give a reduced dose of RUTF to treat a wasted child and still help them recover as effectively. While more research is ongoing to identify the optimal dosage, this update means that there is a potential for huge cost savings in administering RUTF treatment. And increasing the span of a single packet of RUTF means that more children will have access to this resource – which, like any medicine, has a finite supply.
These updates are evidence that progress and reform are possible.
Will Moore, ECF CEO
The updated wasting guidelines were published in two phases. The second section was released on November 20, 2023, and focuses on the prevention of child wasting. The prevention guidelines offer new recommendations on the most effective ways of preventing the occurrence of wasting, including the potential use of specially formulated foods such as small-quantity lipid based nutrient supplements (SQ-LNS) in vulnerable settings. Both the prevention and treatment guidelines have the potential to shift the trajectory for vulnerable children around the world.
ECF CEO Will Moore shared this reflection on the treatment guidelines: “These guidelines are the result of tens of millions of dollars in research that the Eleanor Crook Foundation and other donors have invested to improve malnutrition treatment protocols, and years of hard work and creative thinking from some of the best researchers in our sector. We’re thrilled that many of those improvements are now recommended in the new WHO wasting treatment guidelines. By scaling up these improved approaches, which are now recommended by WHO, we have the opportunity – and the full permission – to make every dollar invested in malnutrition treatment go much further to save children’s lives, and encourage them to thrive. These updates are evidence that progress and reform are possible.”
But while the new guidelines represent a huge milestone in the treatment of children suffering from wasting – and children at risk for malnutrition – we know their true impact is yet to be realized. We look forward to WHO-led efforts to develop a suite of operational guidance, implementation tools, and training to support uptake of the new guidelines at a country level. We also look to key donor agencies to continue to increase financing for wasting treatment and close the funding gap for wasting. ECF estimates that it would take an annual investment of US$ 950 million to fully scale up treatment for severe wasting. Now, more than ever, investment in wasting treatment is a smart buy, representing the latest and most cost-effective innovations that can bring lifesaving treatment to even more of the most vulnerable children.
____
Note: The guidelines review process began in 2019 as part of the Global Action Plan of Child Wasting. The Eleanor Crook Foundation is proud to be one of the funders of this process, along with many others including the Children’s Investment Fund Foundation (CIFF), and UNICEF. WHO has led an intensive review process over these four years, appointing an expert panel to evaluate the latest wasting evidence and to revise recommendations accordingly. As a funder, ECF was an observer throughout the process and had no input in the content of the guidelines.
[1] https://www.who.int/publications/i/item/9789240073791
Photo credit: © UNICEF/UN0724754/Ayene